Dr. Brian Cripe
answers common questions about carpal tunnel release, an effective surgery for treating carpal tunnel syndrome
Finger numbness, tingling, pain, and weakness are all signs of carpal tunnel syndrome, the most common entrapment neuropathy. As a plastic, reconstructive, and hand surgeon, I perform surgery for carpal tunnel syndrome regularly.
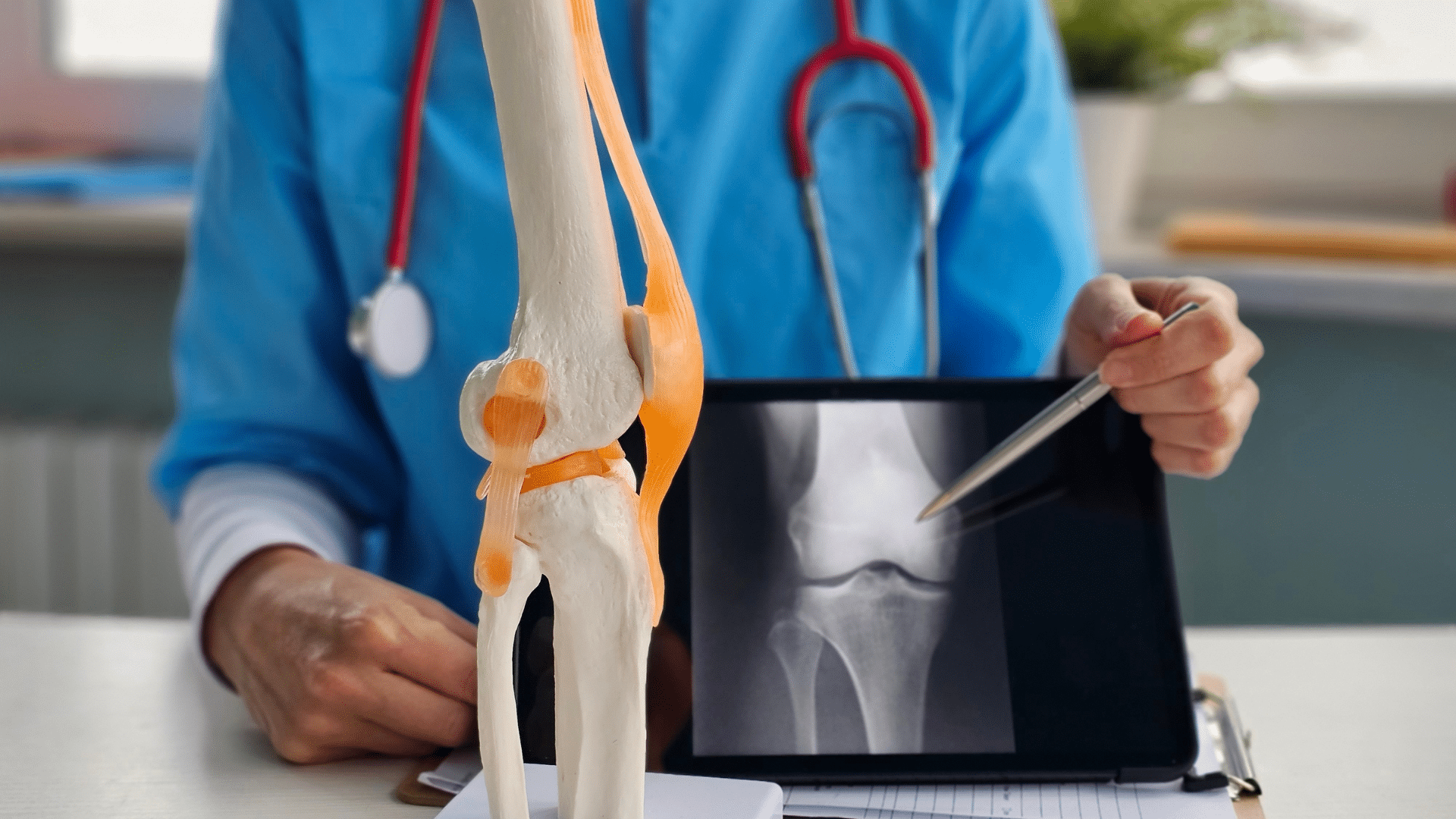
The carpal tunnel is a small passageway made up of bones and ligaments that is located at the base of the hand. When the median nerve becomes compressed or squeezed within the tunnel, it can cause a variety of symptoms such as pain, tingling, numbness, and weakness in the hand and wrist. These symptoms may be worse at night and wake you up from sleep or may be made worse with activities such as driving. Treatment for carpal tunnel syndrome may include rest, wearing a wrist brace, physical therapy, medication, or in severe cases, surgery. When preparing patients for surgery for carpal tunnel syndrome, I often get asked the following questions:
Q: What causes carpal tunnel syndrome?
Common risk factors for developing carpal tunnel syndrome include repetitive hand motions, such as computer work, and underlying medical conditions such as arthritis, diabetes, hypothyroidism, gout, and pregnancy. Carpal tunnel syndrome is due to nerve impingement and can be caused by masses, fractures, anomalous muscle, or swelling of tendons that narrow the nerve canal.
Q: How is carpal tunnel syndrome diagnosed?
Symptoms of CTS can include pain, numbness, tingling, and weakness in the hand and wrist, particularly in the thumb, index, and middle fingers. Pain is usually felt on the palm side of the wrist and hand, but may disperse to other areas. Symptoms are often worse at night or after prolonged use of the hand or wrist. Some patients may notice symptoms more during certain activities, such as holding a phone, writing, typing, or driving. In extreme cases, muscles at the base of the thumb may begin to atrophy causing grip strength weakness and loss of coordination.
During a physical examination for carpal tunnel syndrome, I check for weakness in the hand and wrist, test sensation in the affected fingers, and look for swelling or other signs of inflammation.
I tap over the median nerve at the wrist, which may cause a tingling sensation in the thumb, index finger, long finger, and half of the ring finger – the digits innervated by the median nerve. If the patient does feel tingling, termed the Tinel’s sign, it’s a good indication that they have carpal tunnel syndrome.
We can also use diagnostic tests to confirm a carpal tunnel syndrome diagnosis. These tests include nerve conduction velocity and electromyography studies and can help determine prognosis severity. In our office, we can perform ultrasound examinations to assess the compression of the median nerve. Imaging studies like X-rays or MRIs aren’t typically warranted but may be used to rule out other medical conditions if the patient is experiencing other symptoms in addition to hand numbness and weakness.
Q: How is carpal tunnel syndrome treated?
There are several treatment options for carpal tunnel syndrome depending on the severity of symptoms and how long the patient has experienced them. Severe cases usually require surgery for carpal tunnel syndrome, but mild cases may be resolved with rest and non-surgical treatment techniques.
Resting the hand and wrist is one of the first lines of defense against exacerbating carpal tunnel syndrome. Avoid repetitive strenuous motions – such as typing or texting – that may aggravate the condition. Resting the affected hand helps reduce inflammation and may relieve symptoms. I usually recommend a wrist brace to immobilize the affected hand, alleviating pressure on the median nerve. If you can’t stop the activity, try to scale back repetitive movements and take frequent breaks. Physical therapy, stretching, and strengthening exercises may also improve the condition. I advise patients to make adjustments based on their lifestyle. For example, a patient who works at a desk all day may want to start using ergonomic equipment to help reduce strain on the wrist and hand.
Over-the-counter NSAIDs, such as Aspirin or Ibuprofen, can help reduce inflammation and alleviate pain. Based on the patient, I may inject a corticosteroid directly into the carpal tunnel. This usually provides only temporary relief, but 25% of patients with carpal tunnel syndrome have long-term relief after a steroid injection.
If none of these treatments provide relief, carpal tunnel release surgery is usually recommended.
Q: What does surgery for carpal tunnel syndrome entail?
First, the success rate for carpal tunnel release is very high. The procedure can provide significant and immediate relief of symptoms for my patients.
We perform carpal tunnel release under local anesthesia, sometimes paired with IV sedation, on an outpatient basis. The procedure takes about 15 minutes and you can go home after the surgery.
During the procedure, I cut the ligament over the canal. This takes pressure off of the median nerve and immediately begins to alleviate pain and numbness in the digits. While this procedure can be performed with an open technique, I like to do carpal tunnel release endoscopically to minimize scarring, postoperative pain, and recovery time. For endoscopic tunnel release, I make one small incision at the palm or the wrist to insert a camera and release the ligament while keeping the skin above it intact. Some patients may require an open release, performed with a small incision in the proximal palm.
Q: What does recovery from surgery for carpal tunnel syndrome look like?
After carpal tunnel release, patients can resume their normal activity as pain allows. Patients should open and close their hand 10 times per hour while awake to help encourage healing. I also recommend walking several times a day. Elevating the operative hand, applying cold compresses, and taking Tylenol and Advil can help alleviate pain and swelling. Most patients return to work within 2-7 days after endoscopic carpal tunnel surgery. Some discomfort when putting pressure on the palm is normal for 4-6 weeks after surgery, for example when crawling, pushing out of a chair, or leaning on the hand with the wrist extended.
Surgical dressings can be removed and patients can resume showering after two days. You do not require a splint or cast after carpal tunnel release surgery. Patients should avoid soaking in bathtubs until I clear them. I also advise patients not to swim for six weeks to curb the risk of infection. A small amount of drainage from the incision sites is normal during the first few days after surgery. Patients may find placing clean gauze or absorbent dressing over the incisions can help protect clothing.
Book Your Carpal Tunnel Repair Consultation Today
Our team of board-certified plastic, reconstructive, and hand surgeons at Plastic Surgeons of Northern Arizona can answer your questions and discuss your symptoms and treatment options.