Lipedema is a chronic medical condition characterized by the abnormal accumulation of fat cells, predominantly in the lower extremities, although it can also affect the arms and torso. This condition leads to pain, swelling, and, in some cases, bruising. It is often underdiagnosed but can significantly impact a patient’s quality of life. However, with early diagnosis and appropriate treatment, lipedema patients can manage their symptoms and improve their overall well-being.
What Causes Lipedema?
Lipedema is a chronic loose connective tissue condition characterized by abnormal fat accumulation, primarily in the lower extremities. Despite its prevalence ranging from 10% to 20%, lipedema frequently goes unrecognized and is prone to misdiagnosis. While the exact cause remains elusive, several contributing factors have been identified.
- Hormones: First, the condition predominantly affects women, which suggests a hormonal link as estrogen and progesterone fluctuations may contribute to abnormal fat distributions. Hormonal fluctuations, particularly during puberty, pregnancy, and menopause, are believed to contribute to the onset and progression of lipedema, as estrogen and progesterone fluctuations may impact fat distribution.
- Genetics: Genetics also plays a significant role in the development of lipedema. Research suggests a familial predisposition, indicating that individuals with a family history of the condition may be more susceptible.
- Inflammation: Inflammation is another key element. Chronic low-grade inflammation may disrupt the normal functioning of adipose tissue, leading to its disproportionate accumulation in the lower body. The inflammatory process could be triggered or exacerbated by injury, surgery, or infections.
- Lifestyle Factors: Sedentary behavior and poor dietary habits may exacerbate the symptoms of lipedema but are not considered direct causes. While weight gain often accompanies lipedema, remember that the condition is not solely a result of lifestyle choices. Many lipedema patients I meet have tried to modify their condition with strict dieting and exercise to no avail.
The Science Underlying the Lipedema Disease Process
Lipedema has several key features, including adipocyte dysfunction and adipogenesis, tissue inflammation, altered extracellular matrix components, fibrosis, and fluid accumulation.
Adipocyte hypertrophy refers to the enlargement or increase in the size of adipocytes, the specialized cells that store fat in the form of triglycerides. Adipocytes are found in adipose tissue, commonly known as fat tissue. When an individual experiences weight gain or an increase in fat storage, the adipocytes undergo hypertrophy, expanding their size. In conditions like lipedema, where there is an abnormal accumulation of fat, adipocyte hypertrophy occurs in the affected areas, particularly the lower body. This hypertrophy contributes to the characteristic enlargement of lipedema patients’ subcutaneous adipose tissue. Unlike normal weight gain, where adipocytes can both enlarge (hypertrophy) and increase in number (hyperplasia), lipedema tends to involve primarily hypertrophic changes in the existing adipocytes.
The extracellular matrix is a complex network of molecules that provides structural and biochemical support to the cells within tissues and organs of the body. It is a dynamic and three-dimensional framework composed of proteins, glycoproteins, proteoglycans, and other molecules secreted by cells. Scientists have found that patients with lipedema have fibrotic changes in their extracellular matrix, impacting fat cell composition and function. The role of extracellular matrix remodeling is hypothesized to cause aberrant matrix processing, resulting in fat cell expansion.
Microvascular dysfunction is another potential contributor to lipedema, leading to interstitial fluid accumulation in fatty tissues. Researchers have found disrupted interstitial fluid and tissue volume homeostasis in lipedema models, compromised lymphatic bulk transport, and microangiopathy (small blood vessel dysfunction). Researchers have also shown that certain inflammatory markers, such as immune cell infiltrates and the presence of macrophages, are present in lipedema subcutaneous fatty tissue.
Common Symptoms
Initially a cosmetic concern, lipedema usually progresses over time, causing pain and hindering movement. The legs and buttocks experience continued fat growth, potentially resulting in lymphedema. This condition obstructs the proper drainage of the lymphatic system and can extend to the arms and upper body. Common symptoms include:
- A diminished upper body in contrast to a significantly enlarged lower body, especially the buttocks and legs.
- Legs characterized by a column-like appearance without involvement of the feet
- Bilateral leg swelling and tenderness.
- Unexplained weight gain localized in the lower body.
- Legs that are sensitive and painful, prone to easy bruising.
- Inability to shed weight in the lower body through diet and exercise.
These symptoms can worsen over time and lead to discomfort and decreased mobility.
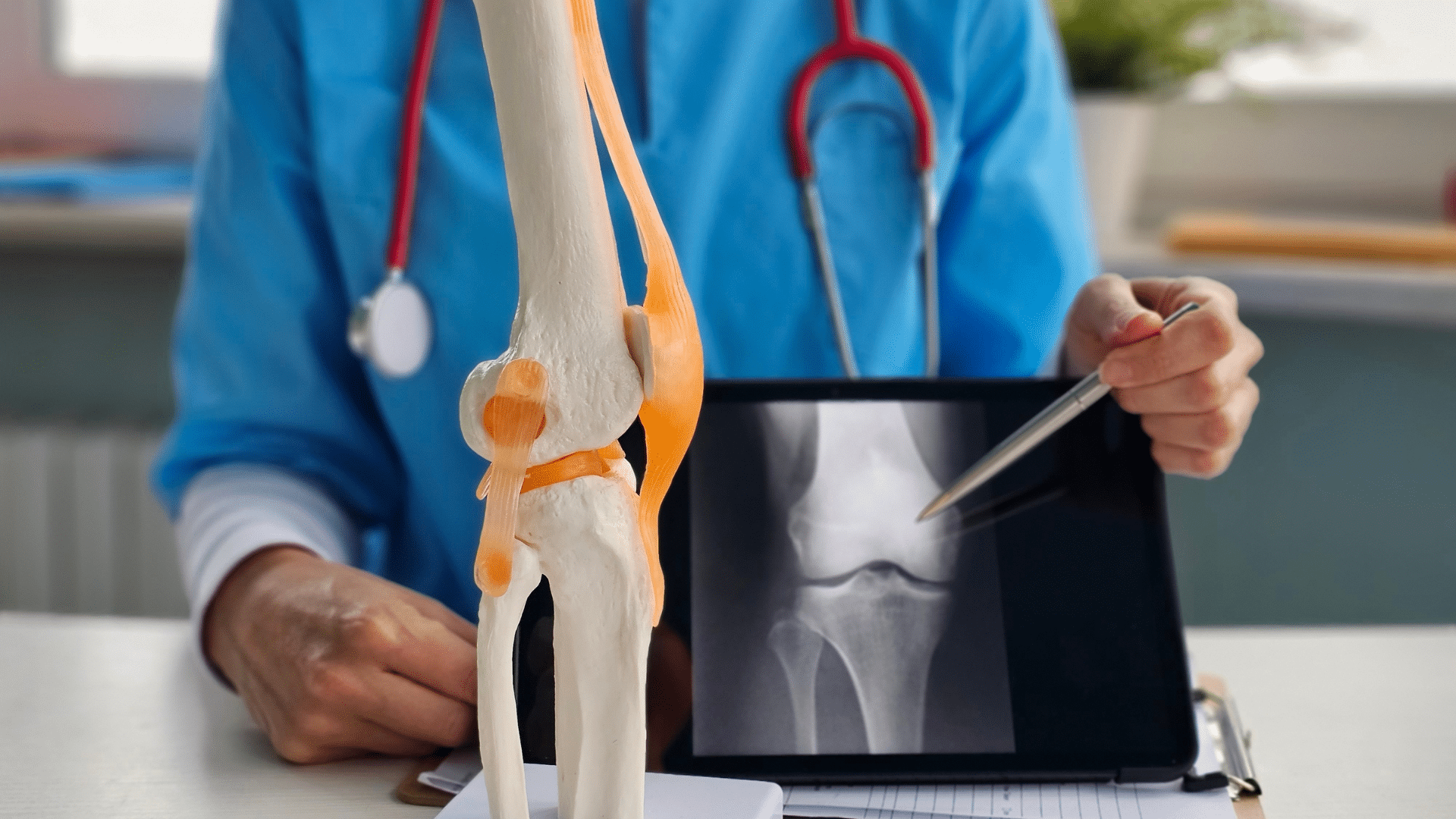
Diagnosing Lipedema
Lipedema is typically diagnosed through a comprehensive evaluation by a specialist. The Lipedema Foundation has made this helpful chart to help practitioners understand differential diagnoses of lipedema and how criteria have changed in recent years. This evaluation may include a physical examination, medical history, and, in some cases, imaging tests to confirm the diagnosis.
Lifestyle Changes
Lifestyle modifications are often recommended to manage lipedema. These include maintaining a healthy diet, engaging in regular, low-impact exercise, and managing body weight to reduce the strain on the affected limbs. The Lipedema Foundation recommends following a low-inflammatory diet and references this book.
Compression garments, such as specialized stockings or sleeves, can be beneficial for managing lipedema. They provide external pressure that helps reduce swelling and alleviate discomfort. Some patients also try mechanical compression via pumps, manual lymphatic drainage massage, and dry brushing to reduce swelling and encourage fluid flow in the affected tissues.
If these conservative treatments aren’t ineffective, the patient may be eligible for surgical interventions.
Lipedema Surgery
Surgery for lipedema can involve multiple different approaches. Liposuction is the surgical procedure most often used to treat lipedema. It involves the removal of excess fat deposits from the affected areas, providing relief from the symptoms. In my experience as a plastic and reconstructive surgeon, liposuction can deliver significant relief for lipedema patients. Some patients require excision of skin and subcutaneous fat, which may also be combined with liposuction.
Here’s an overview of what to expect:
- Patient Evaluation: A thorough evaluation by a board-certified plastic surgeon is essential before considering liposuction. This typically includes a physical examination, assessment of the extent of lipedema, and consideration of the patient’s overall health.
- Preoperative Planning: Your surgeon will develop a personalized treatment plan based on the evaluation. This includes identifying target areas for liposuction, determining the amount of fat to be removed, and assessing the overall goals of the procedure. Additional medical tests may be ordered.
- Anesthesia: Liposuction for lipedema is often performed under general anesthesia or, in some cases, local anesthesia with sedation.
- Tumescent Technique: After anesthesia is administered, we inject a solution containing saline, anesthetic, and adrenaline into the targeted areas. This solution helps numb the area, constrict blood vessels to minimize bleeding, and facilitate fat removal.
- Fat Removal: We insert a thin tube called a cannula through small incisions in the skin near targeted areas. We move the cannula back and forth to break up and suction out excess fat from the affected areas.
- Postoperative Care: Liposuction patients must wear compression garments after the procedure to minimize swelling and support the healing process. Pain management and follow-up appointments are crucial for monitoring recovery. Your surgeon will provide you with compression garments and thorough instructions.
Liposuction results are often noticeable after the initial swelling subsides. Patients typically experience a reduction in the size of the affected areas, improved contour, and enhanced mobility.
Book A Lipedema Consultation in Flagstaff, Arizona
Dr. Brian Cripe treats lipedema patients in Flagstaff, Arizona. Book a consultation today to learn more about your treatment options.
Author Profile: Brian Cripe, M.D., is an award-winning, board-eligible plastic and reconstructive surgeon proudly working with the Plastic Surgeons of Northern Arizona practice. Dr. Cripe specializes in cosmetic surgery, limb salvage, peripheral nerve microsurgery, hand surgery, and oncologic reconstructive procedures. He has performed over 5,000 surgical cases during his nine-year tenure as a surgeon.